|
Integrated service delivery is a major trend right now, intended to create seamless pathways to move people through the health care services they need. Here’s what you need to know about this powerful force in Ontario’s health system. What is Integrated Service Delivery? Integration has been defined as “services, providers, and organizations from across the continuum working together so that services are complementary, coordinated, in a seamless unified system, with continuity for the client.” (Suter, Oelke, Adair, et al, “Health Systems Integration”, October 2007) Integration, as a model, has been implemented as a means and not an end in itself. In other words, integration is usually done in support of a bigger goal, such as better service, improved coordination, efficiency and financial sustainability – not as a goal of its own. In our sectors, specifically, clients are especially likely to face barriers to care. Meeting their needs requires coordinating and integrating community-based health services with acute, mental health, specialized and long-term care, as well as services that address the social determinants of health. Integrating how health care is planned, organized and delivered helps us enhance client care. It’s an opportunity for the health sector to engage effectively with the broader social service sector, ensuring both systems work together in the interest of clients, patients, and our communities. Why Integration Matters Now Ontario is pursuing better quality, seamless patient experiences, and a more cost-effective health system. Integrated service delivery is a key component of the strategy for getting there. For the past several years, Ontario has put integration front and centre, emphasizing integration both between sectors (e.g. primary care to community, home care to CSS, etc.) and between local heath and non-health organizations. Key Types of Integration Although we tend to think of integration in terms of mergers and structural integrations, it can encompass a wide range of practices and approaches. These can include:
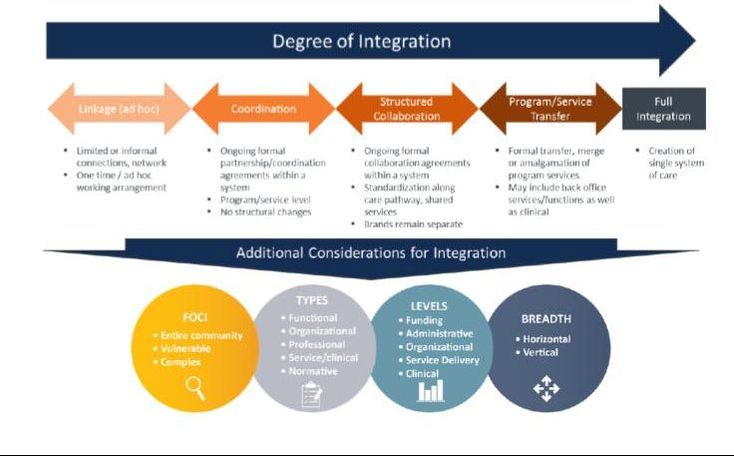
From “Implementing the Integration Planning Program”
Toronto Central LHIN/Optimus SBR, October 7, 2016 The Evolving Role of LHINs in Driving Integration The Local Health System Integration Act (2006) provides LHINs with legislative powers to drive integration through:
Key Resource: CHO Integration Principles While integrating Ontario’s health system is complex, it is important for both the system and its users to keep up our individual efforts. Community Health Ontario’s Integration Principles help all participants -- from the Minister of Health and Long-Term Care to people who use the system and their loved ones -- better address the complexity of the undertaking by working well together. Want to learn more about integration and other key trends in Ontario’s health system? Check out our LeaderShift webinars for Health System Leaders. Comments are closed.
|
https://www.ocsa.on.ca/leadership-in-a-time-of-uncertainty-lessons-from-a-community-care-ceo
|
|
LeaderShift Office:
180 Dundas St. W., Suite 1400-B Toronto, ON M5G 1Z8 |
Subscribe to Our Mailing List
|